Physical & Occupational Therapy
Ready to Get Your Life Back?
Do what you love pain-free with Physical and Occupational Therapy treatment that fits your lifestyle, schedule, and needs.
(716) 458-1990

Your Recovery Journey Starts Here
When pain strikes, trust Buffalo Rehab Group to support you every step of the way. Our Physical and Occupational Therapy services quickly address the root of your pain — and help you get your life back!
Why Choose Buffalo Rehab Group?
We’re not just a therapy provider, we’re your partners on the path to life without pain.
Don’t navigate the fear and frustration of an injury alone. Let’s make your recovery journey — together.
Avoid waiting weeks for an appointment
Start sooner and embrace the freedom of booking where, when, and how you want.
Find a time and place that works for you
With expanded hours across 13 clinics and virtual care, you won’t lose time with family, friends, or work.
Enjoy start-to-finish care
Count on working with the same therapy team throughout your recovery journey.
Get support in and out of the clinic
Access your treatment plan and team through our convenient BRG app.
What Our Patients Are Saying
You Might Be Wondering
How do I schedule an appointment?
To schedule an appointment, please call our Patient Service Center at 716-458-1990. If you wish to chat with a team member or schedule online, you can do so through our website.
What are your hours?
Our standard clinic hours are Monday through Thursday, 7AM to 7PM, and Friday, 7AM to 5PM. Our Patient Service Center is open Monday through Friday, 8AM to 7PM.
Do I need a referral to start treatment?
No, you may begin physical therapy without a referral from your physician. Treatment without a referral is available for 10 visits, 30 days, and with clinicians who have three or more years of experience.
Is my treatment covered by insurance?
Yes, physical and occupational therapy are covered by insurance. Here is a list of health insurance we currently accept.
What can I expect during my first session?
At your initial appointment, your therapist will ask questions and evaluate your range of mobility. Your following sessions will work to treat dysfunction and maximize your recovery through an approach specific to you.
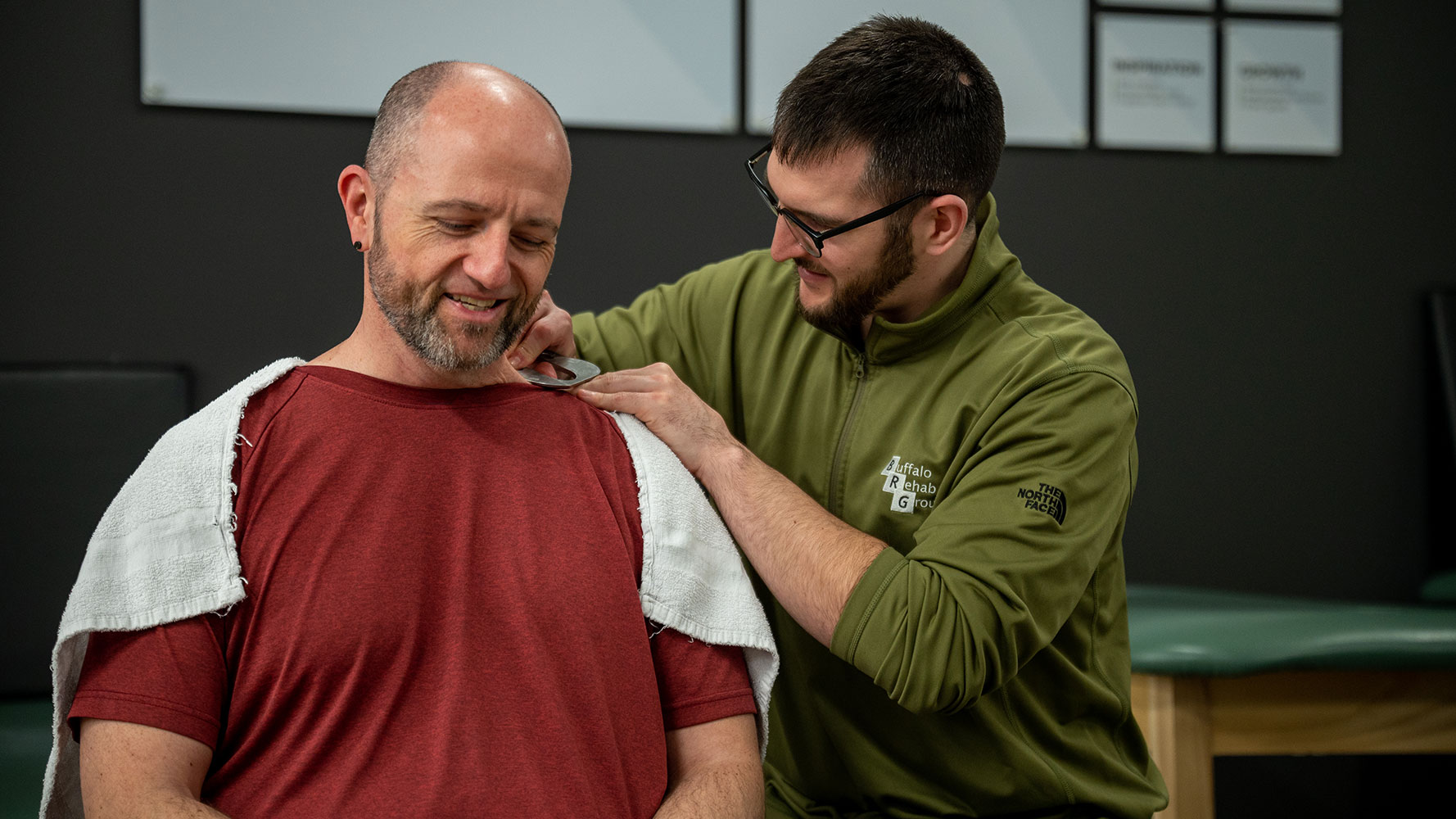
Ready to Move & Feel Your Best?
Get personalized Physical or Occupational Therapy at 13 locations across Western New York or choose our Virtual Physical Therapy option.